1. World Food Prize goes to Sanjaya Rajaram
“The 71-year-old veteran plant scientist has been declared the winner of the $250,000 World Food Prize this week. Born in Varanasi in India and now a citizen of Mexico, he has been chosen for his contribution to increasing global wheat production by more than 200 million tonnes in the years following the Green Revolution.” (2 min read)
2. Tuberculosis bacteria has a chink in its armour
With an increase in the number of antibiotic-resistant bacteria, the need to develop new ways to fight infection has never been more urgent. Now researchers at the Indian Institute of Science have found a new anti-microbial target in TB bacteria, and it holds potential for new drugs. (4 min read)
3. Now we know why drugs don’t work on pancreatic cancer
“The quirks of pancreatic cancer make it one of the most lethal. The survival period after diagnosis is only four to six months. The widely believed reason for this failure has been that in pancreatic cancer, the tissue that surrounds the tumour, called the stroma, blocks the delivery of chemotherapy drugs to the tumour. But new research has turned that logic on its head.” (3 min read)
+ The writer, Mohit Kumar Jolly, is a graduate student at the University of Rice. This week he is blogging from the Lindau Nobel Laureates meeting.
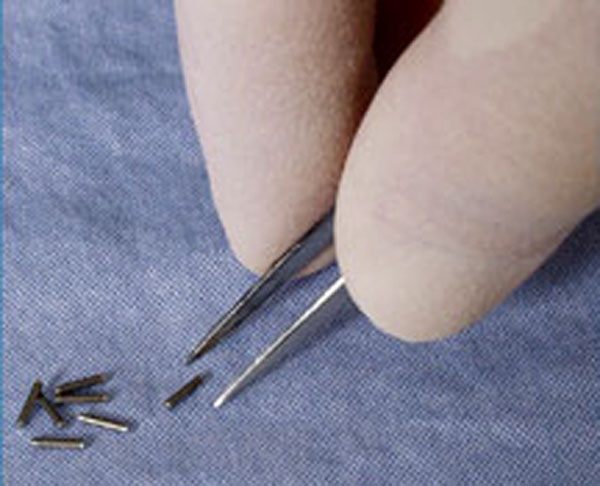
4. The biologist who played with animal poisons
Professor KS Krishnan, one of India’s top biologists, passed away earlier this year. “His fundamental impact was the ease with which he repeatedly linked his questions with the most innovative solutions. He was too smart to pursue science as a set of minor achievable goals. The exciting things he talked about were too broad to be limited to just one discipline. He was a man of science who loved molecules and molluscs in equal measure, researching the unexplored world of animal poisons, looking for that missing miracle cure for some of the most dreaded human diseases of the nervous system.” (3 min read)
5. India’s big brother is coming to Surat
Not the reality TV show, but the Orwellian character who watched over the action of the country’s citizens. Citizens of Surat, however, are celebrating. Their city will become the first to setup a network of closed-circuit cameras. The hope is that it will reduce crime, but past evidence on the use of such networks is not clear. Without proper laws in place to protect citizens’ privacy, India must debate surveillance before it is too late. (4 min read)
Chart of the week
An ageing population is going to be one of the greatest challenges of the 21st century, but solutions around the world differ wildly. Spot India and China in the chart below, and then hope that India’s health minister Harsh Vardhan will start acting rather than creating controversies. Those in the US can weep a little, too. Credit: 2013 health report by the OECD.

For more, follow the curators Mukunth and Akshat. Get in touch with us at curiousbends@gmail.com.